Neuropathy (Peripheral Neuropathy)
Diabetes is a leading cause of neuropathy in the United States, although there are many other causes too. Some cases of neuropathy can be easily treated and sometimes cured. If neuropathy can’t be cured, treatment is aimed at controlling and managing symptoms and preventing further nerve damage.
OVERVIEW
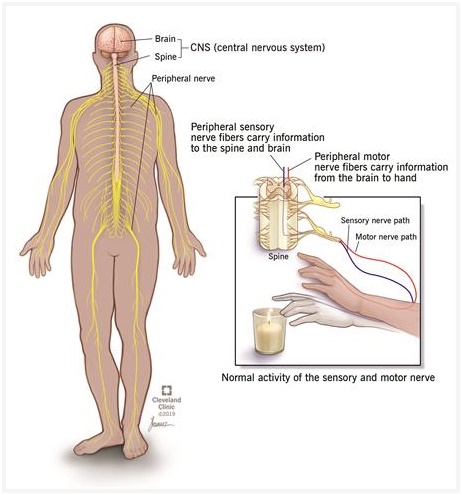
Your peripheral nervous system is made up of the nerves outside your central nervous system. Sensory nerves carry messages to your brain. Motor nerves carry messages to your muscles.
What is neuropathy?
Neuropathy is damage or dysfunction of one or more nerves that typically results in numbness, tingling, muscle weakness and pain in the affected area. Neuropathies frequently start in your hands and feet, but other parts of your body can be affected too.
Neuropathy, often called peripheral neuropathy, indicates a problem within the peripheral nervous system. Your peripheral nervous system is the network of nerves outside your brain and spinal cord. Your brain and spinal cord make up your central nervous system. Think of the two systems working together this way: Your central nervous system is the central station. It is the control center, the hub from which all trains come and go. Your peripheral nervous system are the tracks that connect to the central station. The tracks (the network of nerves) allow the trains (information signals) to travel to and from the central station (your brain and spinal cord).
Neuropathy results when nerve cells, called neurons, are damaged or destroyed. This disrupts the way the neurons communicate with each other and with the brain. Neuropathy can affect one nerve (mononeuropathy) or nerve type, a combination of nerves in a limited area (multifocal neuropathy) or many peripheral nerves throughout the body (polyneuropathy).
What types of peripheral nerves are there and what do they do?
The peripheral nervous system is made up of three types of nerves, each with an important role in keeping your body healthy and functioning properly.
- Sensory nerves carry messages from your five senses (sight, hearing, smell, taste, touch) through your spinal cord to your brain. For example, a sensory nerve would communicate to your brain information about objects you hold in your hand, like pain, temperature, and texture.
- Motor nerves travel in the opposite direction of sensory nerves. They carry messages from your brain to your muscles. They tell your muscles how and when to contract to produce movement. For example, to move your hand away from something hot.
- Autonomic nerves are responsible for body functions that occur outside of your direct control, such as breathing, digestion, heart rate, blood pressure, sweating, bladder control and sexual arousal. The autonomic nerves are constantly monitoring and responding to external stresses and bodily needs. For instance, when you exercise, your body temperatures increases. The autonomic nervous system triggers sweating to prevent your body's temperature from rising too high.
- Chronic headaches
The type of symptoms you feel depend on the type of nerve that is damaged.
What does neuropathy feel like?
If you have neuropathy, the most commonly described feelings are sensations of numbness, tingling (“pins and needles”), and weakness in the area of the body affected. Other sensations include sharp, lightening-like pain; or a burning, throbbing or stabbing pain.
How common is neuropathy? Who gets neuropathy?
Neuropathy is very common. It is estimated that about 25% to 30% of Americans will be affected by neuropathy. The condition affects people of all ages; however, older people are at increased risk. About 8% of adults over 65 years of age report some degree of neuropathy. Other than age, in the United States some of the more common risk factors for neuropathy include diabetes, metabolic syndrome (high blood pressure, high cholesterol, obesity, diabetes), and heavy alcohol use. People in certain professions, such as those that require repetitive motions, have a greater chance of developing mononeuropathies from trauma or compression of nerves.
Among other commonly cited statistics, neuropathy is present in:
- 60% to 70% of people with diabetes.
- 30% to 40% of people who receive chemotherapy to treat cancer.
- 30% of people who have human immunodeficiency virus (HIV).
How quickly does neuropathy develop?
Some peripheral neuropathies develop slowly – over months to years – while others develop more rapidly and continue to get worse. There are over 100 types of neuropathies and each type can develop differently. The way your condition progresses and how quickly your symptoms start can vary greatly depending on the type of nerve or nerves damaged, and the underlying cause of the condition.
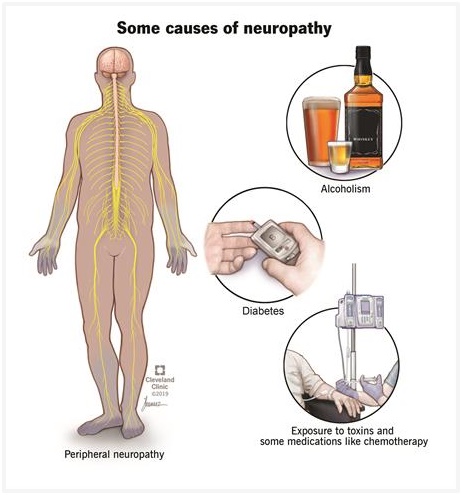
There are many causes of neuropathy. Diabetes is the number one cause in the United States. Other common causes include trauma, chemotherapy, alcoholism and autoimmune diseases.
Symptoms and Causes
What causes neuropathy?
Neuropathy is not caused by a single disease. Many conditions and events that impact health can cause neuropathy, including:
- Diabetes: This is a leading cause of neuropathy in the United States. Some 60% to 70% of people with diabetes experience neuropathy. Diabetes is the most common cause of small fiber neuropathy, a condition that causes painful burning sensations in the hands and feet.
- Trauma: Injuries from falls, car accidents, fractures or sports activities can result in neuropathy. Compression of the nerves due to repetitive stress or narrowing of the space through which nerves run are other causes.
- Autoimmune disorders and infections: Guillain-Barré syndrome, lupus, rheumatoid arthritis, Sjogren’s syndrome and chronic inflammatory demyelinating polyneuropathy are autoimmune disorders that can cause neuropathy. Infections including chickenpox, shingles, human immunodeficiency virus (HIV), herpes, syphilis, Lyme disease, leprosy, West Nile virus, Epstein-Barr virus and hepatitis C can also cause neuropathy.
- Other health conditions: Neuropathy can result from kidney disorders, liver disorders, hypothyroidism, tumors (cancer-causing or benign) that press on nerves or invade their space, myeloma, lymphoma and monoclonal gammopathy.
- Medications and poisons: Some antibiotics, some anti-seizures medications and some HIV medications among others can cause neuropathy. Some treatments, including cancer chemotherapy and radiation, can damage peripheral nerves. Exposure to toxic substances such as heavy metals (including lead and mercury) and industrial chemicals, especially solvents, can also affect nerve function.
- Vascular disorders: Neuropathy can occur when blood flow to the arms and legs is decreased or slowed by inflammation, blood clots, or other blood vessel disorders. Decreased blood flow deprives the nerve cells of oxygen, causing nerve damage or nerve cell death. Vascular problems can be caused by vasculitis, smoking and diabetes.
- Abnormal vitamin levels and alcoholism: Proper levels of vitamins E, B1, B6, B12, and niacin are important for healthy nerve function. Chronic alcoholism, which typically results in lack of a well-rounded diet, robs the body of thiamine and other essential nutrients needed for nerve function. Alcohol may also be directly toxic to peripheral nerves.
- Inherited disorders: Charcot-Marie-Tooth (CMT) disease is the most common hereditary neuropathy. CMT causes weakness in the foot and lower leg muscles and can also affect the muscles in the hands. Familial amyloidosis, Fabry disease and metachromatic leukodystrophy are other examples of inherited disorders that can cause neuropathy.
- No known cause: Some cases of neuropathy have no known cause.
What are the symptoms of neuropathy?
Symptoms of neuropathy vary depending on the type and location of the nerves involved. Symptoms can appear suddenly, which is called acute neuropathy, or develop slowly over time, called chronic neuropathy.
Common signs and symptoms of neuropathy include:
- Tingling (“pins and needles”) or numbness, especially in the hands and feet. Sensations can spread to the arms and legs.
- Sharp, burning, throbbing, stabbing or electric-like pain.
- Changes in sensation. Severe pain, especially at night. Inability to feel pain, pressure, temperature or touch. Extreme sensitivity to touch.
- Falling, loss of coordination.
- Not being able to feel things in your feet and hands – feeling like you’re wearing socks or gloves when you’re not.
- Muscle weakness, difficulty walking or moving your arms or legs.
- Muscle twitching, cramps and/or spasms.
- Inability to move a part of the body (paralysis). Loss of muscle control, loss of muscle tone or dropping things out of your hand.
- Low blood pressure or abnormal heart rate, which causes dizziness when standing up, fainting or lightheadedness.
- Sweating too much or not enough in relation to the temperature or degree or exertion.
- Problems with bladder (urination), digestion (including bloating, nausea/vomiting) and bowels (including diarrhea, constipation).
- Sexual function problems.
- Weight loss (unintentional).
Diagnosis and Tests
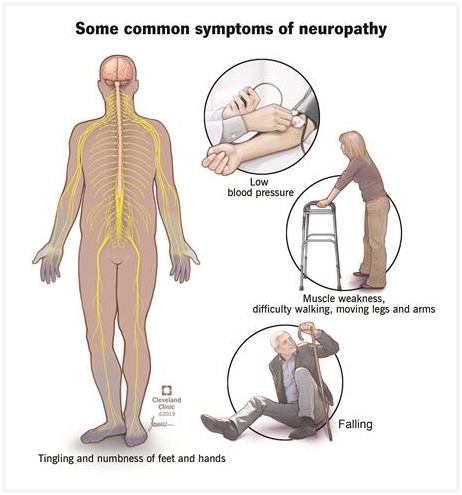
Common symptoms of neuropathy include numbness and tingling, frequent falls, muscle weakness and difficulty walking, and low blood pressure.
How is neuropathy diagnosed?
History and physical exam: First, your doctor will conduct a thorough history and physical exam. Your doctor will review your symptoms and ask questions including your current and past medications, exposure to toxic substances, your history of trauma, your line of work or social habits (looking for repetitive motions), family history of diseases of the nervous system, your diet and alcohol use.
Neurologic exam: During a neurologic exam, your doctor will check your reflexes, your coordination and balance, your muscle strength and tone, and your ability to feel sensations (such as light touch or cold).
Watch out for triggers: Being aware of your child’s diet, activities and medication use can help you find out what usually brings on a headache. Caffeine for example might trigger a headache.
Blood work and imaging tests: Your doctor may also order blood work and imaging tests. Blood work can reveal vitamin and mineral imbalances, electrolyte imbalances (indicator of kidney problems, diabetes, other health issues), thyroid problems, toxic substances, antibodies to certain viruses or autoimmune diseases. Magnetic resonance imaging (MRI) can detect tumors, pinched nerves and nerve compression.
Genetic testing: A genetic test may be ordered if your doctor suspects a genetic condition is causing your neuropathy.
Electrodiagnostic assessment (EDX): Your doctor might send you to a nerve specialist for an EDX to find the location and degree of nerve damage. EDX includes two tests:
- Nerve conduction study (NCS): During this test, small patches – called electrodes – are placed on the skin over nerves and muscles on different parts of your body, usually your arms or legs. A brief pulse of electricity is applied to the patch over a nerve to be studied. The test measures the size of the response and how quickly the nerve is carrying the electrical signal. Both motor and sensory nerves can be studied in this way.
- Needle electromyography (EMG): An EMG can determine the health of a muscle, and determine if there is any disconnection between the nerve and muscle by measuring the electrical activity within the muscle while it is in use. During an EMG, a very thin needle electrode is inserted through the skin into the muscle. The muscle is then used for a specific movement and the electrical activity of the muscle is recorded on a graph called an electromyogram.
Tissue biopsies: In some cases, a nerve, muscle or skin biopsy is needed to confirm the diagnosis. During a biopsy, a small sample of your tissue is removed for examination under a microscope.
Other tests: Other tests include a test to measure your body’s ability to sweat (called a QSART test) and other tests to check the sensitivity of your senses (touch, heat/cold, pain, vibration).
Management and Treatement
How is neuropathy treated?
Treatment begins by identifying and treating any underlying medical problem, such as diabetes or infections.
Some cases of neuropathy can be easily treated and sometimes cured. Not all neuropathies can be cured, however. In these cases, treatment is aimed at controlling and managing symptoms and preventing further nerve damage. Treatment options include the following:
- Medicines : can be used to control pain. A number of different medications contain chemicals that help control pain by adjusting pain signaling pathways within the central and peripheral nervous system. These medications include:
- Antidepressants such as duloxetine or nortripyline.
- Antiseizure medicines such as gabapentin (Neurontin®, Gralise®) and pregabalin (Lyrica®).
- Topical (on the skin) patches and creams containing lidocaine (Lidoderm®, Xylocaine®) or capsaicin (Capsin®, Zostrix®).
- Narcotic medications are not usually used for neuropathy pain due to limited evidence that they are helpful for this condition.
- Physical therapy uses a combination of focused exercise, massage and other treatments to help you increase your strength, balance and range of motion.
- Occupational therapy can help you cope with the pain and loss of function, and teach you skills to make up for that loss.
- Surgery is available for patients with compression-related neuropathy caused by such things as herniated disc in back or neck, tumors, infections, or nerve entrapment disorders, such as carpal tunnel syndrome.
- Mechanical aids, such as braces and specially designed shoes, casts and splints can help reduce pain by providing support or keeping the affected nerves in proper alignment.
- Proper nutrition involves eating a healthier diet and making sure to get the right balance of vitamins and other nutrients.
- Adopting healthy living habits, including exercising to improve muscle strength, quitting smoking, maintaining a healthy weight, and limiting alcohol intake.
Other treatments
- Transcutaneous electrical nerve stimulation (TENS): This treatment involves placing electrodes on the skin at or near the nerves causing your pain. A gentle, low-level electrical current is delivered through the electrodes to your skin. Treatment schedule (how many minutes and how often) is determined by your therapist. The goal of TENS therapy is to disrupt pain signals so they don’t reach the brain
- Immune suppressing or immune modulating treatments: Various treatments are used for individuals whose neuropathy is due to an autoimmune disease. These include oral medications, IV infusion treatments, or even procedures like plasmapheresis where antibodies and other immune system cells are removed from your blood and the blood is then returned to your body. The goal of these therapies is to stop the immune system from attacking the nerves.
- Complementary treatments: Acupuncture, massage, alpha-lipoic acid, herbal products, meditation/yoga, behavioral therapy and psychotherapy are other methods that could be tried to help relieve neuropathic pain. Ask your doctor if any of these therapies might be helpful for treating the cause of your neuropathy.
Prevention
Can neuropathy be prevented?
TYou can reduce your risk of neuropathy by treating existing medical problems and adopting healthy living habits. Here are some tips:
- Manage your diabetes: If you have diabetes, keep your blood glucose level within the range recommended by your doctor.
- Take care of your feet: If you have diabetes or poor blood flow, it’s important to check your feet every day. Look for sores, blisters, redness, calluses, or dry or cracking skin. Keep your toenails clipped (clip straight across the nail); apply lotion to clean, dry feet; and wear closed-toe, well-fitting shoes. Protect your feet from heat and cold. Don’t walk barefoot.
- Declutter your floors. Keep your floors free of items that could cause you to trip and fall. Make sure all electrical cords are tucked away along the baseboards of walls and rooms are well lit.
- Stop smoking: Smoking constricts blood vessels that supply nutrients to nerves. Without proper nutrition, neuropathy symptoms can worsen.
- Maintain a healthy lifestyle: Eat a balanced diet, stay within your ideal weight range, exercise several times a week and keep alcoholic drinks to a minimum. These healthy living tips keep your muscles strong and supply your nerves with the oxygen and nutrients they need to remain healthy.
- Review your medications: Talk with your doctor or pharmacist about all the medications and over-the-counter products you take. Ask if any are known to cause or worsen neuropathy. If so, ask if a different medication can be tried.
Outlook / Prognosis
Can neuropathy be stopped?
Your long-term outcome depends on what is causing your neuropathy. If your neuropathy is caused by a treatable condition, managing the condition might result in stopping the neuropathy or preventing it from getting worse. If the underlying cause of the neuropathy can’t be treated, then the goal is to manage the symptoms of neuropathy and improve your quality of life.
Neuropathy rarely leads to death if the cause is determined and controlled. The sooner the diagnosis is made and treatment is started, the greater the chance that nerve damage can be slowed or repaired. Recovery, if it’s possible, usually takes a very long time -- from months to even years. Some people live with a degree of neuropathy for the rest of their lives.
Can neuropathy be reversed?
If the underlying cause of the neuropathy can be treated and cured (such as neuropathy caused by a vitamin deficiency), it’s possible that the neuropathy can be reversed too. However, frequently by the time individuals are diagnosed with a neuropathy, there is some degree of permanent damage that can't be fixed.
Even though this is the general belief of today, it’s not the hope of tomorrow. Nerve damage may be reversible someday. Researchers are already seeing positive results – the regrowth of nerve fibers – in a drug study in mice with diabetes. Ongoing research combined with living a healthy lifestyle so the body can repair itself will likely be needed. Stay tuned.
LIVING WITH
Can neuropathy lead to amputation?
Yes, neuropathy – especially diabetic neuropathy – can lead to limb amputation. Each year about 86,000 Americans with diabetes lose a limb. The sequence of events leading up to amputation is typically this: the high glucose levels seen in diabetes cause nerve damage. The nerve damage reduces sensation in the limbs (usually the feet), which can lead to unnoticed injuries turning into skin ulcers or infections. Reduced blood flow to the feet, another effect of diabetes, prevents the wound from healing properly. The wounds cause the tissue in the foot or leg to break down, requiring amputation.
You can, however, reduce your chance of an amputation by keeping your diabetes under control and carefully caring for your skin and feet.
What should I do if I think I have neuropathy?
See your healthcare provider immediately as soon as you notice symptoms. Neuropathy can also be a symptom of a serious disorder. If left untreated, peripheral neuropathy can lead to permanent nerve damage.






